Health
Continuous Glucose Monitors Leave Gaps in Diabetes Care
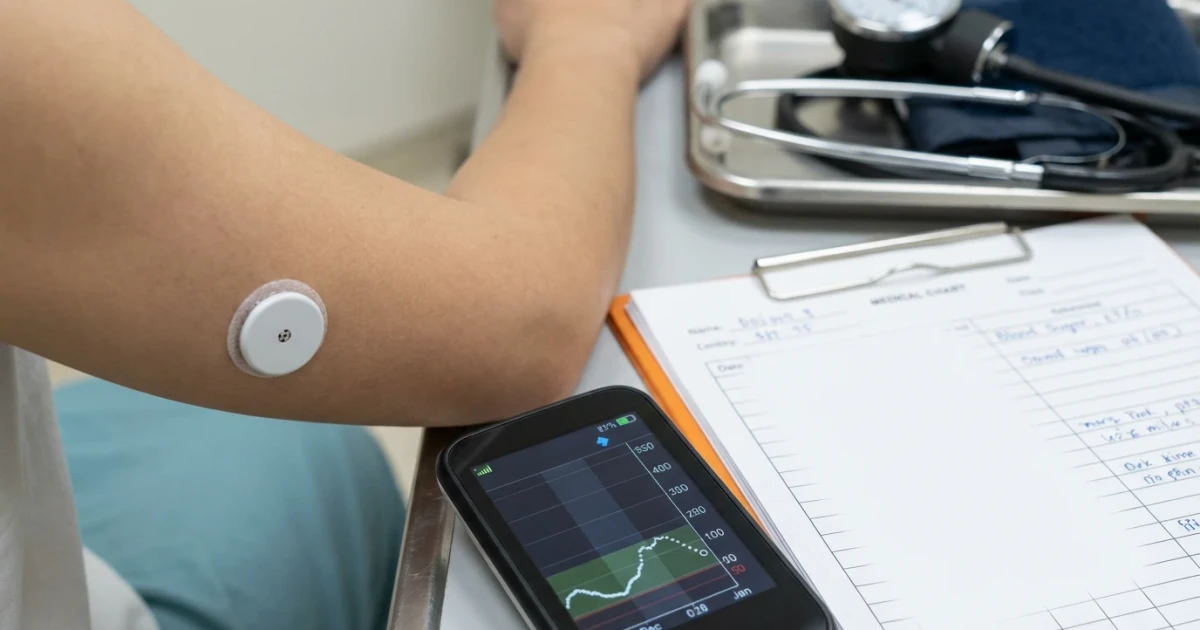
Continuous glucose monitors (CGMs) have revolutionized diabetes management, offering real-time data and convenience for millions. Yet, as highlighted in a recent guest column in The Washington Post, experts studying wearable health data caution that these devices provide only a partial view of a patient’s overall health, potentially overlooking key factors critical to effective care.
CGMs: Transforming Diabetes Monitoring
CGMs track glucose levels in real time, helping people with diabetes manage their condition more proactively. The American Diabetes Association describes CGMs as devices that measure glucose frequently throughout the day, alerting users to trends and sudden changes. For many, this technology means fewer finger pricks and more precise control of blood sugar.
- CGMs have improved glycemic control for users with type 1 and type 2 diabetes.
- They provide valuable alerts for hypoglycemia and hyperglycemia, helping prevent emergencies.
- Adoption rates have increased, with market data showing more Americans using CGM devices each year.
What CGMs Miss: Beyond Glucose Numbers
The Washington Post column underscores that while CGMs are powerful, they are not comprehensive. Wearable health researchers argue that relying solely on CGMs can miss important physiological and behavioral factors that influence diabetes outcomes. For instance:
- Physical activity, sleep, and stress can significantly impact glucose regulation, but CGMs do not directly measure these variables.
- Nutritional intake, medication adherence, and individual metabolic responses are often invisible in CGM data.
- CGMs operate on interstitial fluid readings, which may lag behind blood glucose and be affected by hydration or inflammation.
As wearable health experts note, the context surrounding glucose spikes and dips — such as emotional stress or physical exertion — is essential for understanding what the numbers mean. Without this information, care plans risk being incomplete.
Accuracy and Limitations: A Closer Look
Recent reviews of CGMs, such as the peer-reviewed analysis of their accuracy, highlight common limitations:
- CGMs can have calibration errors and sensor failures, sometimes leading to inaccurate readings.
- Device readings can be affected by environmental factors and user behavior.
- Not all patients respond equally to CGM feedback, especially those with variable daily routines.
Despite these challenges, clinical trials cataloged at ClinicalTrials.gov continue to demonstrate the value of CGMs for improving glycemic outcomes. However, researchers consistently urge caution against relying on CGM data alone.
Integrating CGMs with Holistic Health Data
Wearable health specialists recommend combining CGM data with other forms of monitoring, such as physical activity trackers, sleep logs, and dietary records, for a fuller picture. Integrating these data streams can reveal patterns that single devices cannot, supporting more personalized and effective diabetes management.
For patients and providers, the message is clear: CGMs are a powerful tool, but they are not a substitute for comprehensive health monitoring and individualized care. As technology advances, future devices may offer more integrated data, helping bridge the current gaps.
Looking Ahead
The expansion of wearable health technology presents an opportunity for improved diabetes care, but experts caution against over-reliance on any single device. As adoption grows, understanding the limitations and context of CGM readings will be crucial in supporting both patients and clinicians in making informed decisions.
For now, combining CGM data with other health inputs remains the gold standard for managing diabetes effectively and holistically.